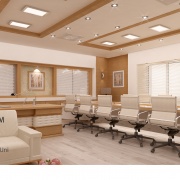
طراحی پلانهای معماری دپارتمان مدیریت بیمارستان نیازمند توجه به چندین نکته کلیدی است که در این پروژه توسط شرکت اسپو انجام شد. در اینجا به برخی از مهمترین این نکات اشاره میکنم:
-
عملکردی و کاربردی بودن فضا: فضاهای مدیریت باید به گونهای طراحی شوند که از نظر عملکردی بهینه باشند. این شامل دفاتر مدیران، سالنهای جلسه و فضاهای مشترک است.
-
دسترسی و ارتباطات: اطمینان از دسترسی آسان به سایر بخشهای بیمارستان و ایجاد ارتباطات مؤثر بین دپارتمانها، از اهمیت بالایی برخوردار است.
-
خصوصیت و حریم خصوصی: فضاهای اداری باید به گونهای طراحی شوند که حریم خصوصی افراد حفظ شود، به ویژه در جلسات مهم و بحثهای حساس.
-
نور طبیعی و تهویه: استفاده از نور طبیعی و تهویه مناسب میتواند تأثیر مثبتی بر روحیه کارکنان و بهرهوری آنها داشته باشد.
-
استفاده از فناوری: طراحی فضا باید قابلیت انطباق با فناوریهای جدید را داشته باشد. این شامل زیرساختهای لازم برای سیستمهای ارتباطی و مدیریتی است.
-
فضاهای استراحت و رفاهی: ایجاد فضاهای استراحت برای کارکنان میتواند به افزایش بهرهوری و کاهش استرس کمک کند.
-
استفاده از رنگ و طراحی داخلی: انتخاب رنگها و طراحی داخلی مناسب میتواند تأثیر مثبت بر روحیه کارکنان داشته باشد و احساس آرامش و راحتی ایجاد کند.
-
قابلیت انعطافپذیری: فضا باید قابلیت تغییر و انعطافپذیری برای پاسخگویی به نیازهای آینده را داشته باشد.
-
مسائل امنیتی: طراحی باید به مسائل امنیتی نیز توجه کند، به ویژه در ورودیها و نقاط حساس بیمارستان.
-
رعایت استانداردها: رعایت استانداردهای مربوط به بهداشت، ایمنی و قوانین ساختمانی در طراحی پلانها بسیار مهم است.
توجه به این نکات میتواند به طراحی یک دپارتمان مدیریت کارآمد و مؤثر در بیمارستان کمک کند.
طراحی نقشههای مکانیکی برای دپارتمان مدیریت یک بیمارستان به منظور تأمین راحتی و کارایی فضاهای اداری بسیار مهم است. در ادامه، به نکات کلیدی و مراحل طراحی این نقشهها اشاره میکنم:
1. تحلیل نیازها
- شناسایی نیازهای حرارتی و برودتی: ارزیابی بار حرارتی و برودتی برای دفاتر، اتاقهای کنفرانس و فضاهای مشترک.
- تنظیمات خاص: در نظر گرفتن نیازهای خاص، مانند سیستمهای تهویه مناسب برای جلسات و فضاهای استراحت.
2. سیستمهای HVAC (گرمایش، تهویه و سرمایش)
- طراحی سیستم HVAC: انتخاب سیستمهای مناسب گرمایش و سرمایش با توجه به نیازهای دپارتمان.
- نقشههای لولهکشی: طراحی مسیرهای لولهکشی برای انتقال هوای گرم و سرد، و تأمین تهویه مناسب.
- انتخاب تجهیزات: مشخص کردن نوع و ظرفیت تجهیزات HVAC.
3. سیستمهای آب و فاضلاب
- نقشههای لولهکشی آب: طراحی سیستم لولهکشی برای آب سرد و گرم به فضاهای مختلف.
- سیستم فاضلاب: طراحی مسیرهای فاضلاب و تأمین دسترسی آسان برای تعمیر و نگهداری.
4. سیستمهای آتشنشانی
- طراحی سیستمهای اطفای حریق: مشخص کردن نوع و محل نصب سیستمهای آتشنشانی و دتکتورهای دود.
- مسیرهای تخلیه: طراحی مسیرهای تخلیه مناسب در مواقع اضطراری.
5. نقشههای جزئیات اجرایی
- جزئیات فنی: ارائه جزئیات فنی برای نصب تجهیزات، اتصالات و لولهکشیها.
- اندازهگذاری دقیق: تعیین ابعاد و اندازههای دقیق برای تجهیزات و لولهها.
6. مدیریت فضا
- استفاده بهینه از فضا: طراحی سیستمها به گونهای که فضای اداری بهینهسازی شود و به نیازهای کاربری پاسخ دهد.
- دسترسی به تجهیزات: اطمینان از اینکه تجهیزات مکانیکی به آسانی قابل دسترسی برای تعمیر و نگهداری هستند.
7. مدلسازی اطلاعات ساختمان (BIM)
- استفاده از نرمافزارهای BIM: مدلسازی سیستمهای مکانیکی برای بهبود هماهنگی با سایر سیستمها و کاهش خطاهای اجرایی.
8. رعایت استانداردها
- انطباق با استانداردها: اطمینان از رعایت استانداردهای ملی و بینالمللی در طراحی سیستمهای مکانیکی.
9. مستندسازی
- تهیه مستندات فنی: ارائه مستندات شامل نقشهها، مشخصات فنی و دستورالعملهای نصب و نگهداری.
10. بررسی و بازنگری
- بازنگری نقشهها: انجام بررسیهای نهایی و اصلاحات بر اساس نظرات و بازخوردهای تیمهای مختلف.
طراحی نقشههای مکانیکی در دپارتمان مدیریت باید به گونهای باشد که به نیازهای کاربران پاسخ دهد و در عین حال ایمنی و کارایی را تضمین کند.
طراحی تأسیسات الکتریکی دپارتمان مدیریت یک بیمارستان نیازمند دقت و توجه به چندین نکته کلیدی است. در اینجا به برخی از این نکات اشاره میکنم:
تحلیل بار الکتریکی: بررسی دقیق بار الکتریکی مورد نیاز برای هر بخش از دپارتمان، شامل دفاتر، اتاقهای کنفرانس و فضاهای عمومی.
منابع تغذیه پایدار: اطمینان از وجود منابع تغذیه اضطراری مانند ژنراتورهای پشتیبان برای مواقع بحرانی.
سیستم روشنایی: طراحی سیستم روشنایی مناسب با توجه به نیازهای مختلف فضا، استفاده از نور طبیعی و انتخاب نورهای LED برای صرفهجویی در مصرف انرژی.
توزیع برق: طراحی سیستم توزیع برق به گونهای که دسترسی آسان و ایمن به پریزها و کلیدهای برق فراهم شود.
سیستمهای کنترل و اتوماسیون: استفاده از سیستمهای هوشمند برای کنترل روشنایی، دما و امنیت به منظور بهینهسازی مصرف انرژی و راحتی کاربران.
مسائل ایمنی: رعایت استانداردهای ایمنی، مانند نصب سیستمهای محافظت در برابر برقگرفتگی و اتصالی، همچنین بررسی نیاز به سیستمهای هشدار و آتشسوزی.
دسترسپذیری: اطمینان از دسترسی آسان به تأسیسات الکتریکی برای تعمیر و نگهداری.
تست و نظارت: طراحی سیستمهای نظارت بر مصرف انرژی و بررسی منظم تجهیزات برای پیشگیری از مشکلات.
آکوستیک و ارتعاش: توجه به مسائل آکوستیک و کاهش نویز ناشی از تجهیزات الکتریکی، بهویژه در فضاهای کار و جلسات.
مدیریت کابلها: استفاده از سیستمهای مناسب برای مدیریت کابلها و جلوگیری از شلوغی و خطرات مرتبط با آن.
توجه به این نکات میتواند به طراحی تأسیسات الکتریکی کارآمد و ایمن در دپارتمان مدیریت بیمارستان کمک کند.